5 shades of nipple discharge
Nipple discharge is not a rare symptom among women who present at breast clinics, which comprise about 5% of the referrals. It is commoner in the ages of 30 – 50 years, mostly among females who have produced offspring and lactated. Fortunately, most of the nipple discharges are not associated with a cancerous lesion deep in the glandular tissues, hence are caused by benign diseases. Therefore it is imperative to understand how the gravity of the diagnosis could change with shades of nipple discharge.
Checking for nipple discharge is also an essential part of ‘breast self-examination’ (BSE), which has been recommended to be done by women monthly, commencing from around 20 years. But it is important to appreciate that BSE is not a screening test for breast cancer.
Nipple discharge is detected by ladies either when notice stained undergarments (spontaneous discharge) or during self-examination. But proper inspection of the discharge should be done by examining in front of a mirror with adequate light. In addition to shades of nipple discharge, it is important to check whether the discharge occurs from both breasts or is it the same extent on both sides and is it from a single or multiple ducts?
When self-check for a nipple discharge, it is important to assess the position of the nipple, whether it has inverted and for any associated nipple rash. The nipple should be squeezed at the base to express a discharge. If only a blob of discharge appears at the tip of the nipple, is usually due to a single duct discharge rather than multiple close by duct openings.
Physiological discharge
There are instances of physiological nipple discharge that occur related to the changes in the hormonal milieu of the female reproductive system. The earliest such discharge can be seen at birth with the release of neonatal prolactin, with the change that occurs from the maternal circulation to their neonatal hormonal environment. Prolactin is an adult female hormone that normally produces milk in the lactating breast. Likewise, neonatal prolactin which can secrete at birth irrespective of the sex of the newborn can increase the blood flow to the neonatal underdeveloped duct and lobules producing a scanty nipple discharge, termed ‘witch’s milk’. It is not scientifically advisable in attempting to perform old-fashioned bewitchments during this normal, transient and physiological phenomenon.
It is not uncommon for a middle-aged woman, who has breastfed before to have slight discharge from the nipple/s occasionally. It is due to damaged and dilated ducts (Duct ectasia) with a stagnation of fluid within them. But if the discharge is from a single breast and particularly from a single duct, it is a sign to obtain immediate medical attention.
Similarly, a physiological insignificant nipple discharge can be seen within the menstrual cycles due to hormonal change, which can go unnoticed.
The shades of nipple discharge is one of the important indicators that the woman should pay attention to.
- WATERY
A colourless watery nipple discharge is a sign that usually does not need to worry. It could occur from one side or both, and single or multiple ducts. A scanty watery discharge can be physiological as explained above. Further at the beginning of pregnancy, there could be a watery type of discharge which become more whitish shade later, closer to delivery.
Fibroadenosis, fibrocystic disease are some of the vague terms used to describe a benign breast condition where structural damage, scarring (fibrosis), cysts formation occurs concurrently probably due to hormonal change. Further due to damaged and dilated ducts (duct ectasia) with the stagnation of fluid, can lead to a watery discharge either from a single duct or multiple and from both sides. This is a benign condition without any risk of further progressing to cancer.
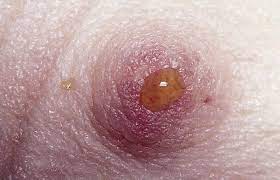
2. STRAW COLOURED
A turbid or straw shade of nipple discharge could be due to further progression of benign conditions such as fibroadenosis or duct ectasia. The prolonged and continued damage of breast tissues makes the discharge a darker shade.
3. BROWNISH DISCHARGE
The brownish or sometimes a greenish discharge is due to associated infection of the fluid which has collected within the ducts following scarring and structural damage to the glandular tissues. It is important to differentiate a brownish seepage from an absolute bloody discharge as most women get panicked with the turbid, brownish colour. Further brownish colour can occur in a benign condition called periductal mastitis, which is seen among the younger women who smoke. The toxins found in tobacco tends to alter the normal bacterial flora, which results in overgrowth of unusual and atypical organisms leading to these darker shades of nipple discharge. Unless an abscess is formed, the use of antibiotics and reassurance usually suffice in controlling the condition.
4. MILKY DISCHARGE
Milky discharge is commonly seen during pregnancy and lasts slightly longer after cessation of breastfeeding. If not, a milky discharge is considered pathological and needs to be investigated. As milk secretion is controlled by a hormone called prolactin, an excess of it could lead to a milky discharge from the nipple. Growth in the pituitary gland in the brain which is formed by cells that secretes prolactin called a prolactinoma should be always excluded when a woman present with the abnormal secretion of milk from the nipple. Blood investigation to estimate the serum prolactin levels usually helps to confirm the diagnosis. In addition, the milky discharge could occur as a side effect of certain medications such as antidepressants, antipsychotics, sedatives, some drugs used to control gastritis and high blood pressure.
5. BLOODY DISCHARGE
Bloody discharge, either a drop or copious, should be investigated as it is the most sinister sign of all discharges. Affecting one breast and a single duct is more significant. Almost 90% of bloody discharges are associated with a benign condition called duct papilloma, which has the potential to become cancer later. Although it is not common for breast cancer to present with bloody nipple discharge, a bloody discharge should be considered always due to cancer until proven otherwise.
Investigations
The shade of nipple discharge is the most important sign clinicians consider in the initial workout in arriving at a diagnosis. Investigations such as breast ultrasonography, a mammogram for women over 40 years can follow after proper examination of the breast is done. Although it is not routinely requested, in special circumstances an MRI may provide additional information. The secretion smeared onto a slide to reveal the cellular pattern (cytology) is rarely performed due to its low sensitivity now.
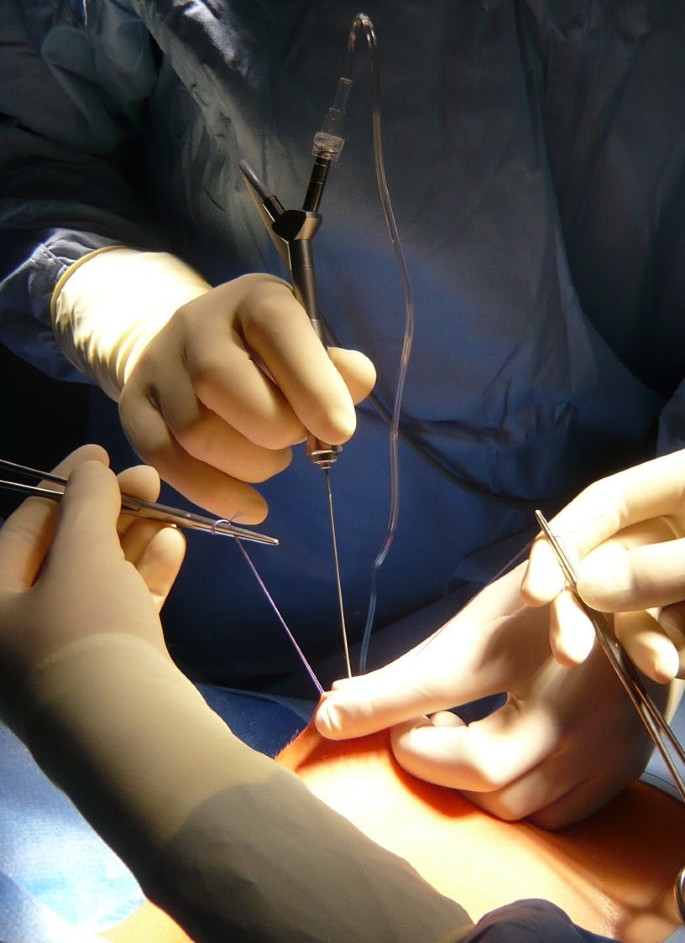
Ductoscopy, using a microendoscopy is a novel approach to investigate and treat all nipple discharges. The miniature endoscope is passed into the offending duct after slight dilatation, allows direct visualization, cleaning of any debris within the duct and has the potential to biopsy any abnormal growths.
Treatment
Removal of the duct/lobular unit, especially when it is suspicious of cancer is known as microdochotomy. It can be performed under local or general anaesthesia and through a small periareolar incision. There aren’t any major complications of this surgery and will not affect breastfeeding in the future.
Suggest further reading…
https://cancerinsrilanka.com/breast/7-features-that-a-breast-lump-could-be-cancer
Ductoscopy video



